What Makes a Measurement-Based Care Platform Effective?
- Why Many Measurement-Based Care Platforms Fall Short
- What Actually Makes an MBC Platform Effective
- Making Patient Feedback Easy to Capture and Sustain
- Turning Data Into Insight—Not Just Information
- Supporting Clinical Decision-Making in Real Time
- Fitting Seamlessly Into Clinical Workflows
- Connecting Measurement to Outcomes and Organizational Value
- How Greenspace Health Supports Effective MBC
What Makes a Measurement-Based Care Platform Effective?
The most effective Measurement-Based Care (MBC) platforms go beyond collecting patient-reported outcomes—they automate assessment delivery, integrate into clinical workflows, and provide real-time insights that clinicians can use to guide treatment. Platforms that fail to support these capabilities often create additional administrative burden without improving care.
Why Many Measurement-Based Care Platforms Fall Short
As Measurement-Based Care continues to gain traction across mental health, more organizations are adopting tools that promise to support outcome tracking and data-driven care. But in practice, implementation doesn’t always translate into impact.
In many cases, organizations encounter familiar challenges. Assessments are completed inconsistently, data is difficult to interpret, and clinicians struggle to incorporate results into sessions in a meaningful way. Over time, this creates friction, both for clinicians and for patients, and MBC risks becoming something that is done alongside care, rather than something that actively contributes to it.
The issue isn’t the intent behind Measurement-Based Care. It’s whether the technology supporting it is designed to make that data usable in real time.
What Actually Makes an MBC Platform Effective
In practice, the effectiveness of an MBC platform comes down to a small number of capabilities that determine whether data is consistently collected, clearly understood, and actively used in care. The most impactful platforms tend to share a common foundation:
- They make it easy to capture patient feedback without adding administrative burden
- They present data in a way that clinicians can quickly interpret and act on
- They surface signals that help identify risk, lack of progress, or disengagement early
Without these elements, even well-designed MBC programs can struggle to influence clinical decision-making.
Making Patient Feedback Easy to Capture and Sustain
One of the most immediate barriers to effective MBC is consistency. If assessments are not completed regularly, the data quickly becomes fragmented and less useful.
To address this, leading platforms prioritize automation. Assessments are delivered at the right time, reminders are built in, and the process requires minimal effort from both clinicians and patients. This ensures that data collection becomes a reliable part of care, rather than something that depends on manual follow-up.
Over time, this consistency is what allows organizations to move from isolated data points to meaningful trends.
Turning Data Into Insight—Not Just Information
Collecting data is only the first step. For MBC to have an impact, clinicians need to be able to quickly understand what that data is telling them.
Effective platforms support this by making trends visible and intuitive. Rather than requiring clinicians to interpret raw scores, they provide clear views into how patients are progressing over time, where improvement is occurring, and where it may be stalling.
In practice, this means clinicians can spend less time interpreting data and more time using it to guide conversations and treatment decisions.
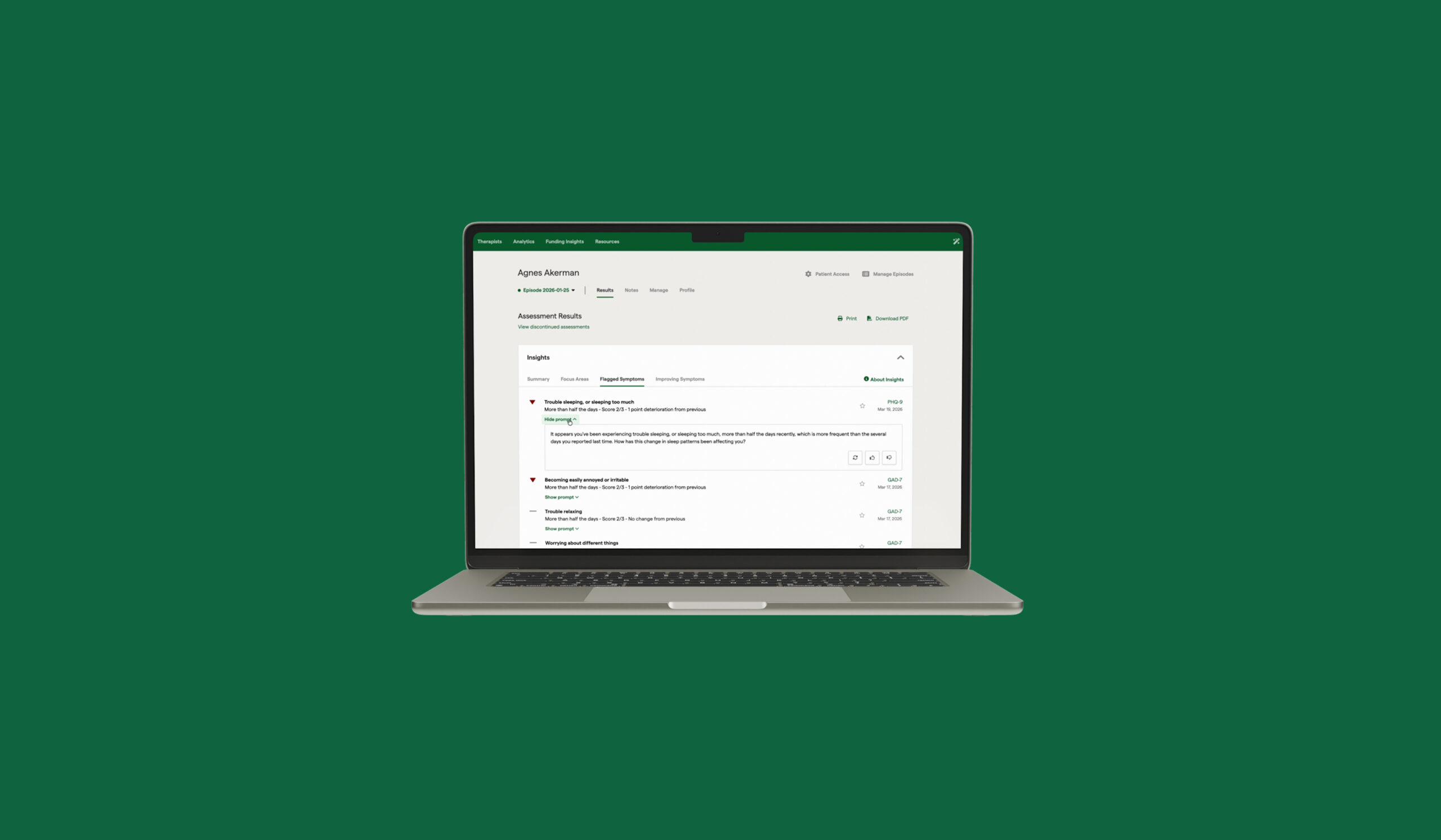
Supporting Clinical Decision-Making in Real Time
The most meaningful impact of MBC comes when it influences what happens in the room. This requires more than visibility—it requires guidance.
Leading platforms help bridge this gap by surfacing signals that might otherwise be missed, such as:
- Early indications that a patient is not improving as expected
- Patterns that suggest increasing risk or deterioration
- Signs of disengagement that could lead to dropout
By making these signals visible in real time, clinicians are better equipped to adjust care earlier, rather than reacting after issues have escalated.
Fitting Seamlessly Into Clinical Workflows
Even the most advanced MBC tools will fall short if they sit outside of the clinician’s day-to-day workflow. When platforms require additional logins, manual processes, or extra steps, adoption naturally declines.
This is why integration is critical. The most effective platforms are designed to fit within existing systems and workflows, making it easy for clinicians to access and use data without disruption. When MBC is embedded into the flow of care, it becomes a natural part of the clinical process rather than an added task.
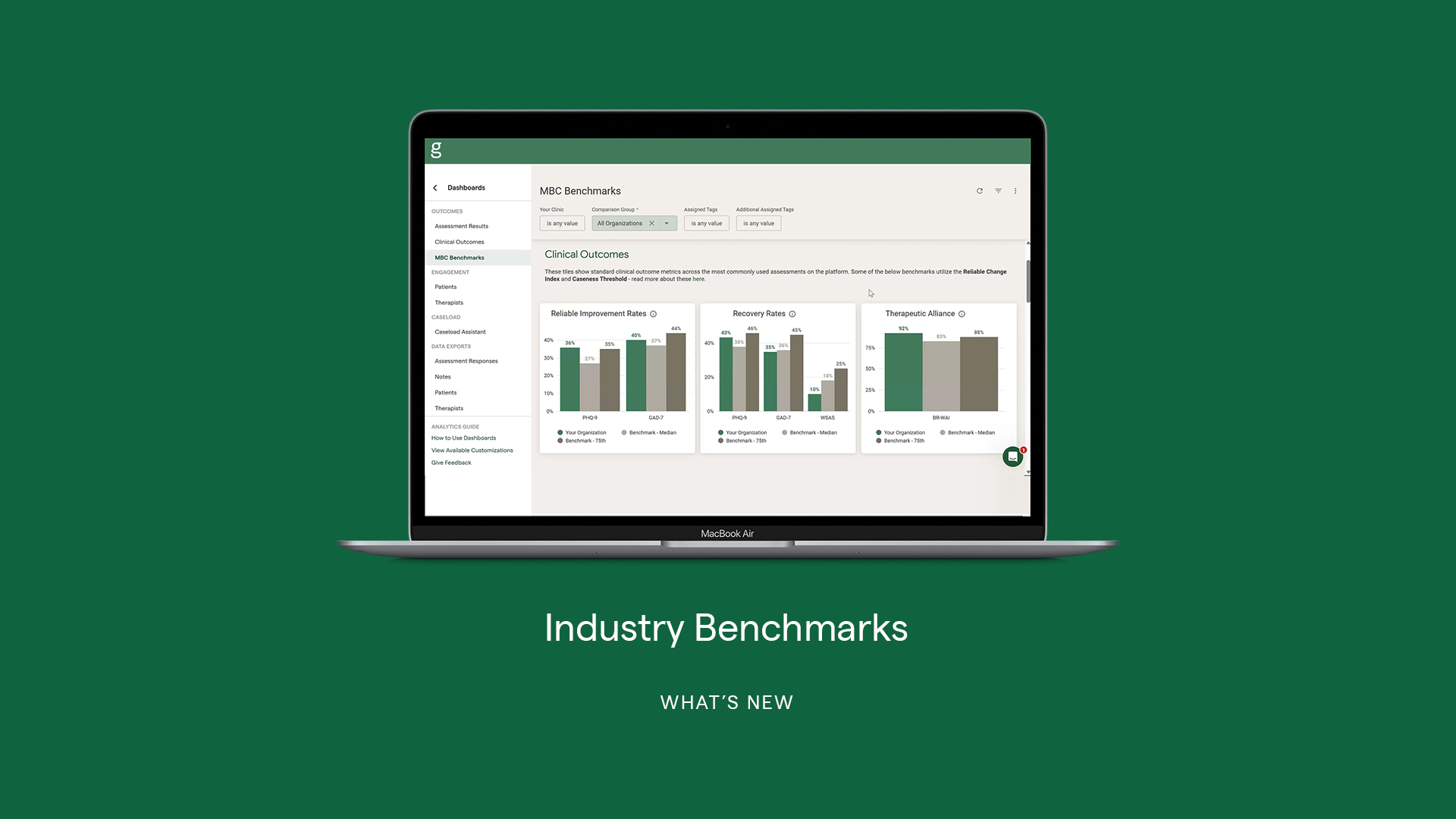
Connecting Measurement to Outcomes and Organizational Value
Beyond individual care, MBC plays an increasingly important role at the organizational level. As mental health continues to shift toward outcomes-based models, the ability to demonstrate impact is becoming essential.
When implemented effectively, MBC enables organizations to:
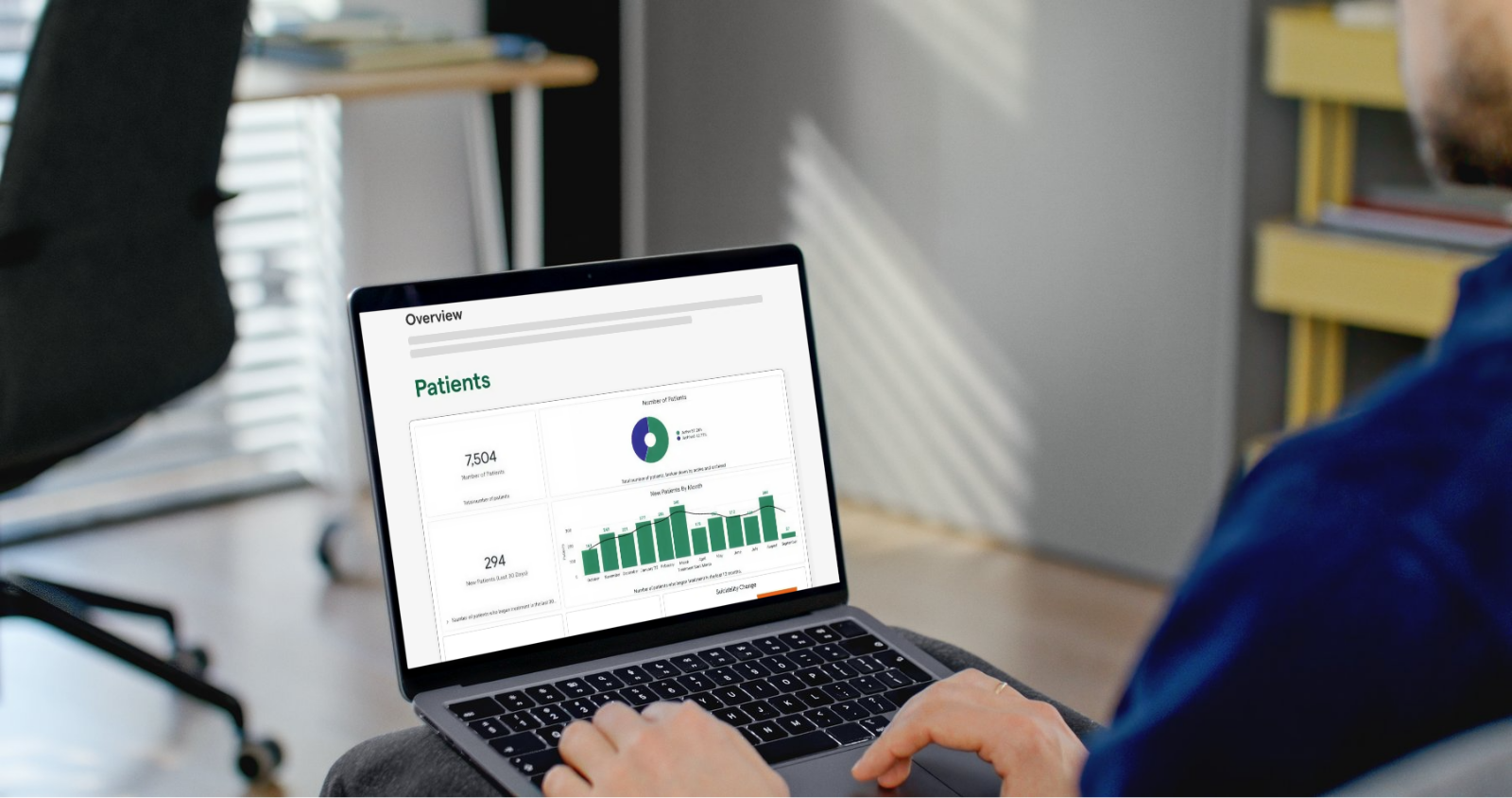
- Track outcomes across programs and populations
- Identify opportunities for quality improvement
- Support conversations with payers, funders, and accrediting bodies
This is where measurement moves beyond clinical utility and becomes a strategic asset.
How Greenspace Health Supports Effective MBC
Greenspace Health is designed to help organizations move beyond data collection by embedding measurement directly into care delivery.
By automating assessment delivery, integrating into clinical workflows, and providing real-time insights, Greenspace enables clinicians and organizations to consistently use data to guide care. At the same time, robust reporting and benchmarking capabilities support broader organizational goals, from quality improvement to value-based care readiness.
The result is a model where measurement is not an added burden, but a core component of how care is delivered and improved over time.
Final Takeaway
Measurement-Based Care is not defined by whether data is collected, but by whether that data is used.
When platforms make it easy to capture, interpret, and act on patient-reported outcomes, MBC becomes a powerful tool for improving care. When they don’t, even well-intentioned efforts can struggle to deliver meaningful impact.
As expectations around outcomes, accountability, and value continue to evolve, the ability to operationalize MBC effectively will only become more important.