Sparking the movement towards Measurement-Based Care (MBC) isn’t just about creating technology platforms to empower clinicians and their clients to easily implement MBC; one of the most influential ways we can work to help encourage the adoption of MBC is by creating engaging educational opportunities with the worlds brightest minds who often work behind the scenes, driving the progress of MBC. That’s why we’re thrilled about our new educational partnership with the Yale Measurement-Based Care Collaborative (The Collaborative), a group of renowned psychologists who have dedicated their careers to its advancement.
To introduce you to The Collaborative’s four faculty members prior to our first panel, we interviewed each of them asking about their perspectives and experiences surrounding MBC, and its value in defining the future of behavioral health services.
Let’s start from the very basics, what is MBC?
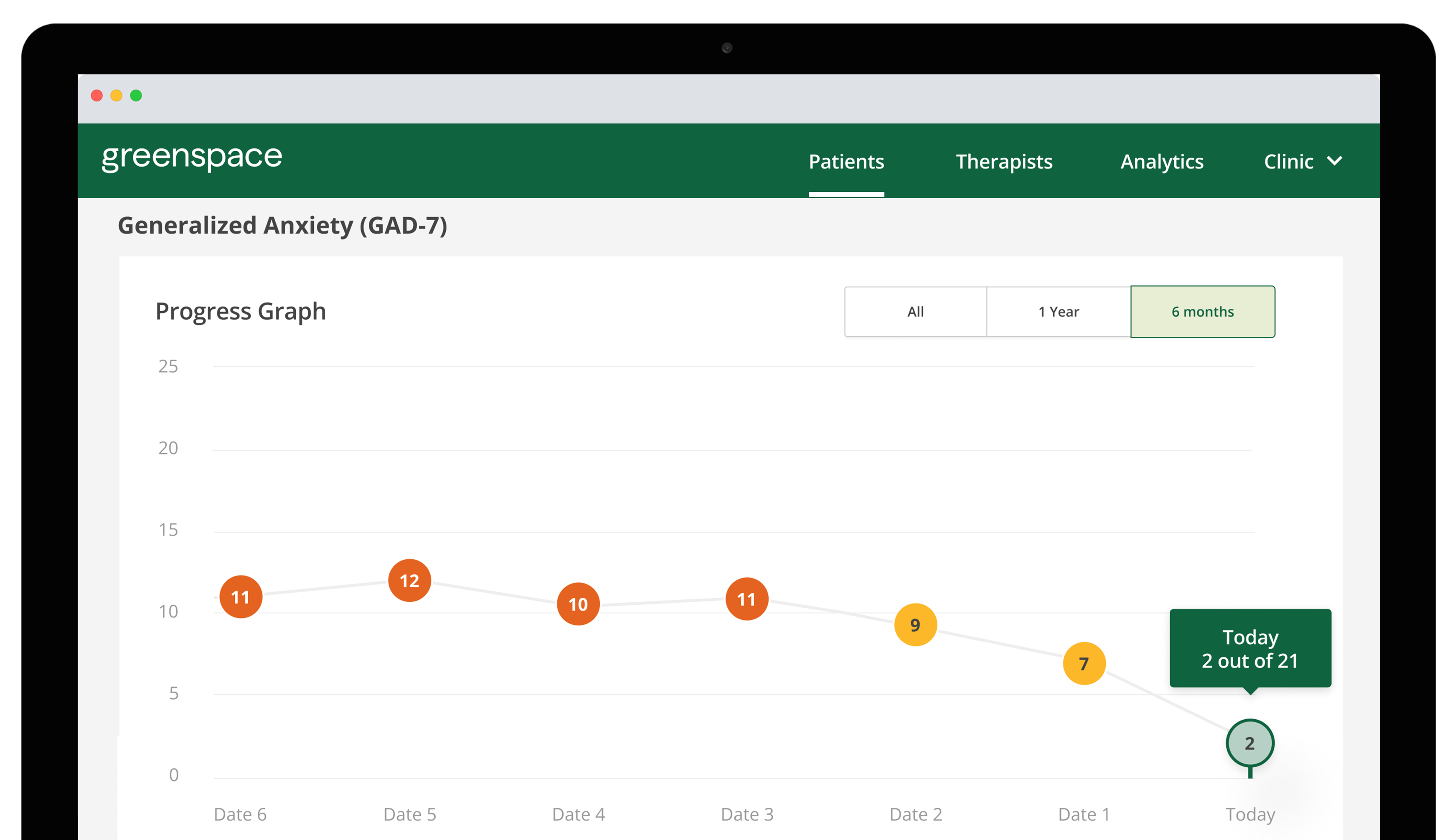
Sandy: MBC is a clinical process that uses patient-reported outcome measures over time to track process and serve as the foundation for important collaborative conversations between clients and providers. We use “collect, share, act” to describe each important step in the process.
Amber: What Sandy said! I tell teenagers that MBC is… “using data about what you say is happening, to get curious about your treatment and our work together. We’re going to use that information to work as a team and make decisions about how we’re going to solve problems and what happens next.”
Elizabeth: Sandy is right on! Amber raises a great point that we need to use client-friendly language when explaining MBC. I encourage clinicians to tell children and families that MBC is a way to track progress together, so everyone is on the same page about our goals, what’s working and what should be adjusted along the way.
Jessica: I’ll just add that by using MBC, we’re inviting clients to reflect on their progress on a regular basis. It’s a way of reminding them (and us) to pause and check in: How am I doing right now? It’s so easy to forget to do that when we get swept up in the processes of mental health treatments (and life). Many of my clients tell me that they use completing the measures as their way to self-assess and to organize their thoughts for our sessions, which is an added bonus.
Why have you chosen to make MBC research and implementation such a significant part of your career?
Amber: MBC helps to improve patient outcomes. Simple as that! So, naturally, I think everyone should use MBC, but unfortunately, that’s just not what is happening in daily practice. Demonstrating the value of MBC to clinicians (research) and developing and studying processes to take the guesswork out of making MBC work in practice (implementation) are important areas of focus for my work.
Elizabeth: I’ve always loved the power of meaningful, actionable data that people can use to describe their experience of mental health services and improve outcomes for children and families. As an evaluator, trainer and consultant, data reviews with providers and care teams always open conversations about stakeholder experiences, the context, and why data look the way they do. With MBC, client progress data are just one piece of the puzzle, and how we make sense of the data is where the truth lies. MBC was a perfect fit for me because it integrates data as one tool to center client experiences and empowerment in their own care.
Sandy: Although I’ve always been an MBC practitioner, I only started working on an MBC implementation project because of my experience in leading large scale dissemination efforts. It wasn’t until I really started to dig in that I realized how completely aligned it was with my beliefs and values about mental health care. My career has always been focused on using data and evidence-based care to improve patient-centered mental health systems, and MBC was a perfect marriage between these two big important concepts – data and patient-centeredness – that have always been important to me.
Jessica: MBC has been a part of my practice since my days as a trainee, and hopefully I’ve been able to pass that on to the trainees I have supervised over the years. When an opportunity came up that would allow me to support a national effort, I couldn’t refuse. MBC is something any mental health professional can use and when done well, it has clear benefits, and I want to help as many people experience those as possible.
Tell us about how you think MBC helps people in care.
Amber: As a person working primarily in the youth space, I think MBC “flips the script” on how teenagers think that care is going to move forward. Youth I’ve worked with are used to adults getting to be in the driver’s seat if you will, about so many aspects of their lives, including mental health care. After all, it’s usually the case that a grownup has brought them into treatment or decided that they needed support, rather than the other way around. MBC is a way of communicating that the process is going to be a shared process and that what the youth says about their experience actually matters. I think it can go a long way for buy-in with this group.
Jessica: My favorite MBC experiences happen when clients realize improvement they weren’t aware of. At times, even when things remain difficult, MBC can help us see progress that would have otherwise flown under the radar. That leads to discussions about what is working or going well for a client, which builds confidence and hope. These are MBC magic moments!
Elizabeth: I think there is still a lot of confusion and mystery in the general public about what mental health services are and how they work. This lack of transparency perpetuates stigma and is disempowering because the client arrives, and the clinician is then in the expert role to “do their thing”. If it’s not a good fit for the client, the only option is to terminate care. MBC really breaks down this dynamic because there is full transparency about the treatment goals, how progress will be measured, the active role of the client to provide feedback, and how decisions will be made about treatment.
Sandy: In so many ways! Completing patient-reported outcome measures helps people better understand themselves and what goals they want to accomplish in treatment. It’s a way of knowing themselves through repeated assessment and empowering people to be partners in their care. It also helps providers know when treatment isn’t working, which leads to important conversations with people about their goals and how to get there. This improves outcomes.
How does MBC help support clinicians?
Sandy: Clinicians talk to us about how they learn more about their clients through the MBC clinical process than they do without it. The structure of “collect, share, act” helps clients develop a language to talk about their experiences and it gives providers so much more information than they might have using open-ended questions alone.
Elizabeth: The clinicians I work with tell me that MBC produces clinical information they would not have otherwise known. Sometimes, the client’s ratings or experience are not what they would have expected, and that is golden.
Jessica: MBC is immensely versatile. We can monitor symptoms, functioning, quality of life, treatment satisfaction, alliance, and more. This versatility means MBC can be folded into virtually any treatment or psychotherapy. What other clinical process has the potential to benefit such a wide range of clinicians and clients?
How will MBC help improve the overall quality of mental and behavioral health services?
Elizabeth: The typical behavioral health provider in “usual care” services delivers eclectic therapy, meaning they use their training, knowledge of the evidence, and experience to individualize the treatment plan and sequence to each client. MBC offers a continuous quality check to evaluate the effectiveness of those individualized plans for each client, and signal when adjustments are needed to optimize results.
Sandy: There’s a ton of research showing that as providers we’re really terrible in predicting how well someone will do in treatment, and we’re similarly not so good at noticing a lack of improvement in care. MBC helps provide signals to providers that what we’re doing isn’t working, and gives us a chance to change things up and try something else, all informed by the preferences and goals of the clients.
Amber: Without a doubt, when used well, MBC takes the goal of individualizing treatment to a whole new level! When we can tailor treatment and goals according to the person receiving services, we might improve engagement and overall outcomes.
What about MBC excites you the most?
Jessica: I want everyone I work with to feel like an active and empowered partner in their care and to always understand what we’re doing and why. MBC is central to achieving that.
Sandy: I love how MBC gives clients a simple entry point for collaboration with their mental health provider. MBC gives clients a way to assess their progress in reaching their goals, and a routine space for them to share their perspectives with providers on how treatment is going.
Amber: I really believe in the value of centering and elevating the voices of the people who we serve, and letting their experiences be what guides our work together. At the core, MBC is about what the patient says is important to them. What could be more powerful than empowering others to be active partners in their own wellness?
Elizabeth: MBC can be added to basically any treatment plan, service modality, or client to individualize care, engage clients and improve quality. This is a practice we need to double down on!
There you have it, an introduction to the incredible team behind the The Yale Measurement Based Care Collaborative, and their high level thoughts on the impact of MBC.
Related Resources