Client engagement is one of the most powerful components of the therapeutic process and plays a crucial role in treatment outcomes. There are countless different approaches to mental health treatment options; however, none will be successful if the client is not engaged.
Measurement-Based Care (MBC) allows clients to take an active role in their treatment and enables them to better understand their progress. Not only does it encourage their active engagement, it also contributes to a stronger therapeutic alliance with their therapist.
What is Client Engagement?
Engagement in mental health treatment involves a healthy therapeutic relationship between client and clinician, characterized by active participation and collaborative decision-making throughout treatment. Engaging clients is essential in order for treatment to lead to positive outcomes. Engaged clients are also clients who feel safe, supported, and comfortable to speak freely with their clinician.
So, How Does MBC Improve Client Engagement?
There is plenty of research illustrating the power of MBC in promoting client engagement. It does this by empowering clients with the knowledge, skills and confidence to better understand their mental health, take an active role in their treatment process and experience improved outcomes. MBC helps to enhance client engagement in 3 key ways: (1) Visibility into assessment results and treatment progress, (2) collaborative decision-making, and (3) improved client-clinician communication. These factors not only result in a stronger therapeutic alliance, but they’re also essential in ensuring that clients have agency in their treatment process. Let’s explore these 3 qualities in more depth below.
1. Visibility Into Assessment Results and Treatment Progress
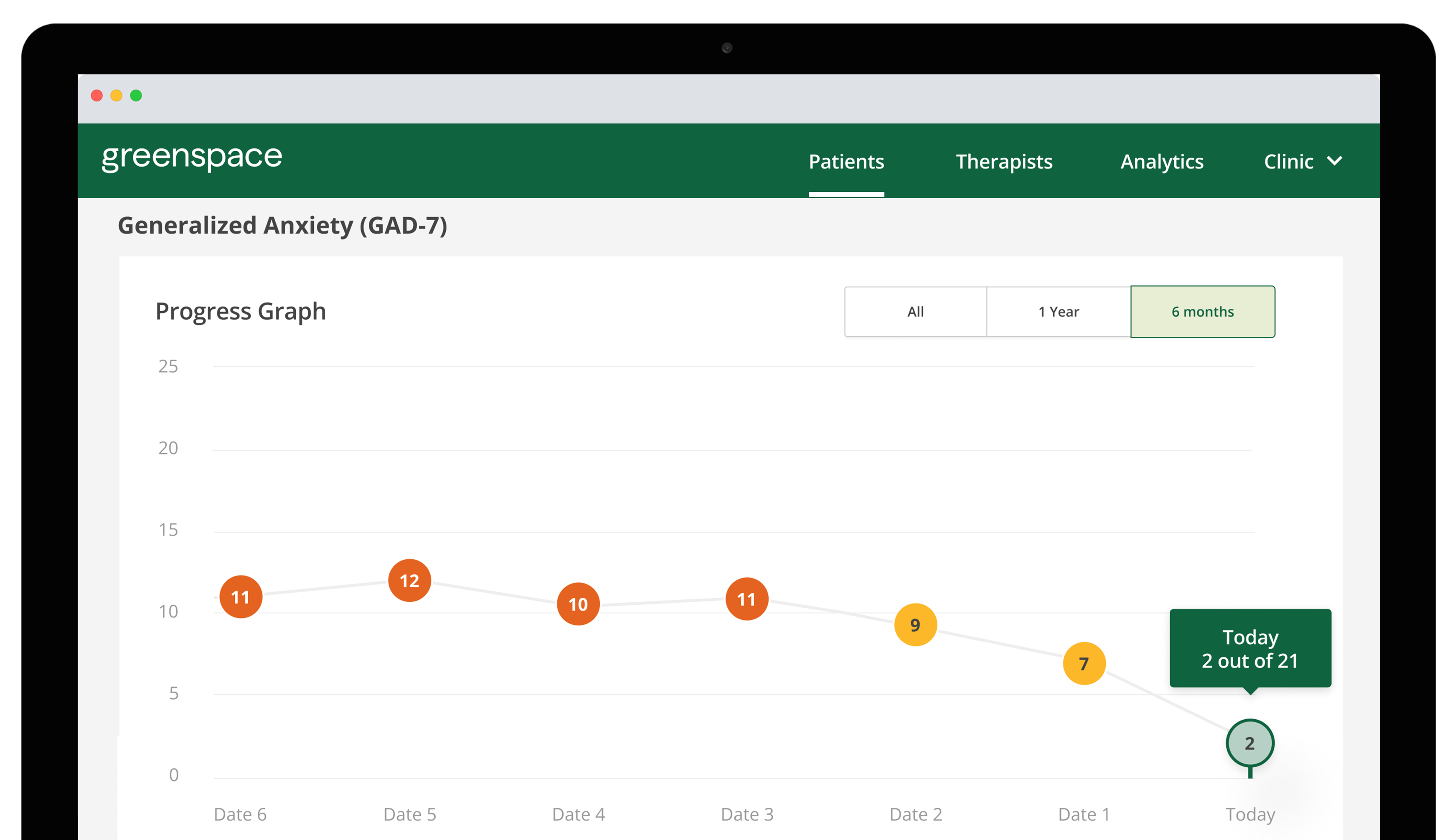
MBC enhances engagement in therapy by allowing clients to have full visibility into their treatment progress, leading to a stronger overall understanding of their mental health journey. Studies consistently show that when clients regularly complete self-reported rating scales they are more likely to become knowledgeable about their mental health concerns, attuned to the fluctuation of their symptoms, and become more aware of warning signs of relapse or recurrence (Fortney et al., 2018). They can become experts on their unique journey, symptoms and therapeutic goals, which helps eliminate the stress that may come with a sudden change in condition.
“We found that it [MBC] was a really good way to focus clients on a session. Some clients are difficult to engage and so with incorporating the assessments, it really helped. They really enjoyed seeing the progress they made, or if they weren’t making progress, you know, understand the ups and downs.”
— Lisa Serfass, LCPCRegional Director at Villa Maria Behavioral Health Catholic Charities Child & Family Services
With the help of data visualizations, clients have the ability to recognize their own improvement throughout treatment, which may have gone unnoticed without tracking progress. Even small improvements in symptoms can empower clients to feel hopeful and motivated, leading to improved engagement and commitment to their therapeutic process.
2. Collaborative Decision-Making
Treatment outcomes are strongest when clients are actively involved in treatment decisions. Providing people in care with access to data that speaks to their treatment results makes it easier for them and their clinicians to recognize when treatment isn’t working and when changes in therapeutic approach may be needed.
As clients become more involved in treatment decisions, they will feel empowered to take more ownership of their care process. The transition from passively receiving care to being an active participant in care is essential; when decisions are made collaboratively, engagement is higher, there is less drop out, higher satisfaction and better outcomes. When clients are actively involved in their treatment process, outcomes are at their best.
3. Improved Client-Clinician Communication
Empowering clients with the skills and confidence to better communicate with providers may be the most powerful change to make towards improved therapeutic outcomes. Whether treatment is going well or not, it’s important for a client to be able to share their thoughts that may prompt changes to the treatment plan and lead to improved outcomes.
In cases where a client may not share information verbally, clinicians can rely on patient reported outcomes that are provided through the implementation of MBC. That data will provide a more detailed picture of what the client is experiencing and will help create an opportunity for the clinician to open up a meaningful dialogue about the client’s perspective and treatment progress. The clinician can vocalize what the client may not be able to, further validating their feelings and strengthening therapeutic alliance.
Wrapping Up
Clients are in the best position to inform the treatment process by assessing their overall symptoms and progress towards treatment goals, which can be easily accomplished through regular client report assessments. Giving clients agency in their care through MBC and allowing them to better understand and communicate about their own mental health is key to ensuring they remain actively engaged in the therapeutic process and see improvement in their outcomes.
If you are interested in learning more about MBC and how it can increase engagement and improve clinical outcomes, you can book a call with one of our implementation experts or send us an email anytime at info@greenspacehealth.com.
Related Resources